CONTACT YOUR PHYSICIAN IF YOU HAVE CONERNS ABOUT STOPPING THERAPY. We may need to collect diagnostic data without the use of therapy. If you have used PAP therapy for an extended period, it may be difficult for you to sleep without it during your sleep study. Taking a short break may help us collect the data necessary for your physician to proceed with the next step.
How to Prepare for Your Study
We want your stay to be as comfortable as possible. Advanced notification can help us better prepare your night if you require additional resources or assistance. IE-caregiver/translator accommodations, head support, restroom proximity, early or daytime appointment. Call or Contact Us
It is important to collect data that closely resembles how you would normally sleep in your own bed. Caffeine may limit the amount of sleep you obtain during your test and alcohol may alter the results of the study.
It is important to collect data that closely resembles how you would normally sleep in your own bed. Several medications can an influence sleep quantity and quality. You should take what your physician has prescribed for you.
Monitoring pulse rate and blood oxygen level is an important tool for assessing sleep disorders. This sensor uses light to obtain values. Nail polish may affect the way this sensor is designed to work.
(What to Expect)
Tech will answer all questions
Hotel room atmosphere
Tech monitors from different room
Tech applies sensors
Only doctor can discuss diagnosis
May be connected to PAP therapy
Testing will end at 6:00am
Arrive on time
Sensors and electrodes will be connected to the scalp
What to Bring to Your Sleep Study
Personal Items Such As Books, Magazines, Tablets
Pajamas And Sleeping Attire
Toiletries
Photo ID
Insurance Card

A sleep study monitors your brain waves, breathing, heart rate and body movements while you sleep. It is performed in our sleep lab by a trained Sleep Technologist. The results of your sleep study will enable your doctor to correctly assess your sleep concerns.
On the day of the study, you will usually be asked to arrive at the sleep lab in the evening. The Technologist will attach sensors to your head, chin, chest, and legs. The technologist will monitor the activity transmitted by the sensors throughout the night. They may ask you to change positions in order to collect the most accurate data. This is a vital part of the process.
Your doctor may have ordered a “split-night study” if you are at a risk for obstructive sleep apnea. If you show signs of sleep apnea during the first half of the study, then the Technologist may apply Continuous Positive Airway Pressure (CPAP) therapy during the second half of the night. CPAP provides air pressure through a mask that opens the upper airway during sleep. Sometimes it may be hard to obtain a clear representation of your sleep disorders during the first part of the study and a second study is needed to complete the process. Despite our best efforts to make you as comfortable as possible, the autonomic nervous system is in control while you are sleeping.
The sleep study ended by 6:00am and removal of the sensors only takes a few minutes.
No, the sleep study is not painful, but the Technologist may ask you to try to sleep on your back during the study. Please inform the Technologist if sleeping on your back is uncomfortable.
Most people do not have difficulty sleeping during the study. If you do have trouble falling asleep, medication may be used to help you. Here at California Sleep Solutions, we do not administer or prescribe any medication. Even if you are unable to sleep the entire time, you will likely sleep long enough for your doctor to make a diagnosis.
We are not able to accommodate guests in our facilities beyond 11:00 PM, except for guardianship purposes or for care giving. Please contact our office at least 72 hours in advance to make arrangements for care givers.
Yes, you can use the restroom in the sleep center. The Technologist can easily disconnect the wires so that you can go to the bathroom privately.
Yes, be sure to bring any medications Modafinil that you take at bedtime. Please let the Technologist know about the medications before you take them.
Generally, it is required for you to try to sleep in the bed. Sleeping in an elevated position in a recliner may affect the results of the study. We do have wedges for you to sleep under if needed.
We have a hotel like setting with large queen or full beds that have firm tops for a better night sleep.
If you receive CPAP therapy during the second half of the study, the sleep Technologist will help you get used to the treatment. The sleep Technologist may try more than one type of mask or make other adjustments to help you feel more comfortable.
One of our board-certified sleep physicians will review the data that we collect during the night and send their recommendations to your physician. The results of your study should be sent to your physician in about two weeks. If your physician doesn’t contact you with the results, you may want to give them a call to schedule a follow up appointment. Your sleep study will also be uploaded to OnPatient for you to view.
Yes, you should wear loose unrevealing night clothing that will allow access to your chest and lower legs.
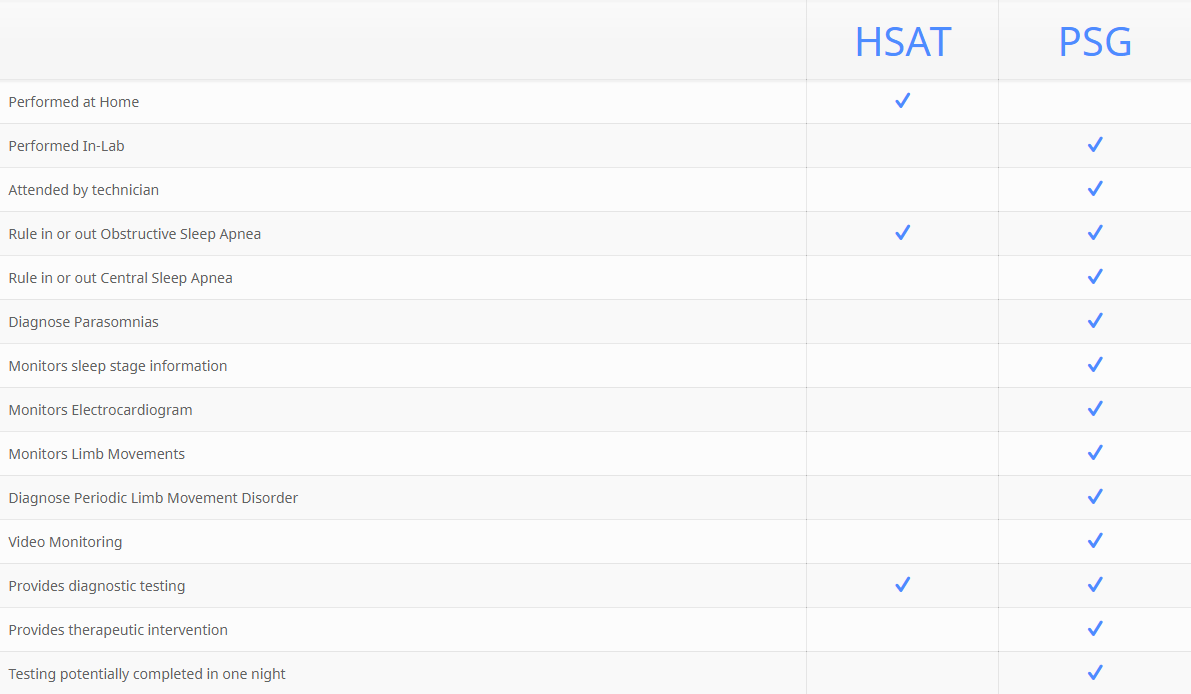
An overnight PSG with PAP Titration, if patient meets insurance criteria. Utilized to gather data for diagnosis & treatment of sleep disordered breathing in a single night study.
Daytime monitoring of the patient following to measure alertness during the day.
An overnight test utilized to gather data for the diagnosis of obstructive sleep apnea in the patient’s home. This test is not recommended for all patients.
An overnight test, typically prescribed for seven days, utilized to gather data for the treatment of sleep disordered breathing in the patient’s home.
A single overnight test utilized to monitor oxygen levels in the patient’s home.